One of the main challenges the industry of radiology currently faces is AI integration. Every day, researchers publish new state-of-the-art algorithms, detecting all sorts of diseases, but how do we bring this valuable research to the clinic? Firstly, the algorithms need to be incorporated into user-friendly software packages which need to obtain regulatory approval. However, it does not end there; an essential requirement for software usability is radiology workflow integration.
Radiologists are not very eager to add yet another stand-alone software solution to their tool set. This raises a challenge. Although there are many other ways of AI integration, each approach has its own advantages and disadvantages. This article discusses the pros and cons of 5 levels of integration for image-based AI, going from manual to full AI integration.
1. Minimal (or should we say manual?) AI integration
Installing the AI software on a workstation would give the radiologist access to AI results. However, without further integration, this just bluntly adds another software program that needs to be opened alongside other software, either on the same computer, or, perhaps, even on a separate workstation. The benefit is clear; it is a very easy-to-realize integration by solely having to install the AI radiology software. Just imagine it as going to a website, downloading the software package, and running it. Done. However, radiologists need to either manually add the AI results to their report (how error prone can you be?), or add the results as an appendix - far from user-friendly.
An example: a separate workstation for AI integration
The most straight-forward example of this kind of integration is with a separate workstation. An extra computer dedicated to automated AI analyses will be installed in the reading room. An example of the related radiology workflow is shown in figure 1. This is neither very integrated nor very efficient - radiologists can only access the AI software if they are physically present at the dedicated workstation. Additionally, the workstation cannot be used by multiple radiologists concurrently. However, this type of integration can offer the radiologist a great level of control. The software can be designed in such a way that AI results can be adjusted, validated, and complemented - if desired. If a hospital has a very high workload of a specific type of scans, a dedicated workstation might be the right option. Additionally, for institutes granting significant autonomy to radiographers, allowing them to generate AI-based reports and forward them to the picture archiving and communication system (PACS), a separate workstation can be the right solution.
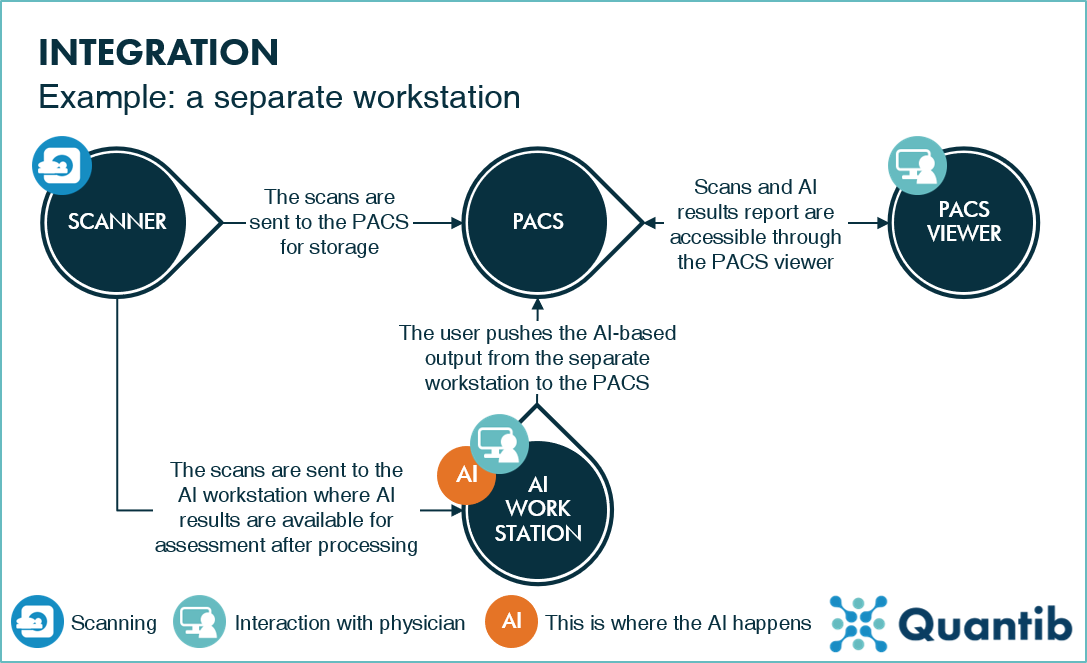 Figure 1: An example of a radiology workflow involving a separate AI workstation. In the most common set-up, the scanner sends the results directly to the AI workstation, which processes the scans, from which the AI-based output can be forwarded to the PACS, where the results are stored and accessible through the PACS viewer.
Figure 1: An example of a radiology workflow involving a separate AI workstation. In the most common set-up, the scanner sends the results directly to the AI workstation, which processes the scans, from which the AI-based output can be forwarded to the PACS, where the results are stored and accessible through the PACS viewer.
2. Fully automatic AI integration
Making fully automatic results from AI radiology software accessible from other systems is a slightly more integrated way of AI implementation. Please pay attention to the words “fully automatic”; the results are generally returned to either PACS or radiology information system (RIS) as a fixed report, meaning there is no option to edit or validate. This AI integration is very easy to use, because radiologists do not have to prepare anything, and the results automatically appear in the PACS as soon as the AI solution has finished processing.
If it suits your reporting to add the AI results to the radiology report as an appendix, or if the results are merely an input to the final report, it can be the right solution for you. However, the lack of editing options can be a downside. Many AI solutions provide standardized reports which are designed to be easy to interpret, also by clinicians; sometimes the reports even include normative reference values providing context to the AI results. Hence, the reports are very suitable to forward to referring physicians for use as additional input for the diagnosis. In this situation, however, the algorithm performance is extremely important. As the process does not include a (manual) check by the radiologist, the software needs to show outstanding results.
An example: a node for AI integration
A hospital can install an automatic processing server as a node in their own network. An example of a workflow including such a node is shown in figure 2. One can think of a node as a separate box that performs AI analyses and returns the results to another system that is part of the radiology workflow. Usually, the PACS receives scans from the scanner, forwards them to the node, which processes the scans and creates a report. Finally, the node returns the report to the PACS in DICOM format, accessible through the PACS viewer. The template of the report is set, there is no option to edit or validate results. It is important to keep in mind that the PACS is an archive, meaning that once a report is saved in the PACS, it is not easy to change or remove.
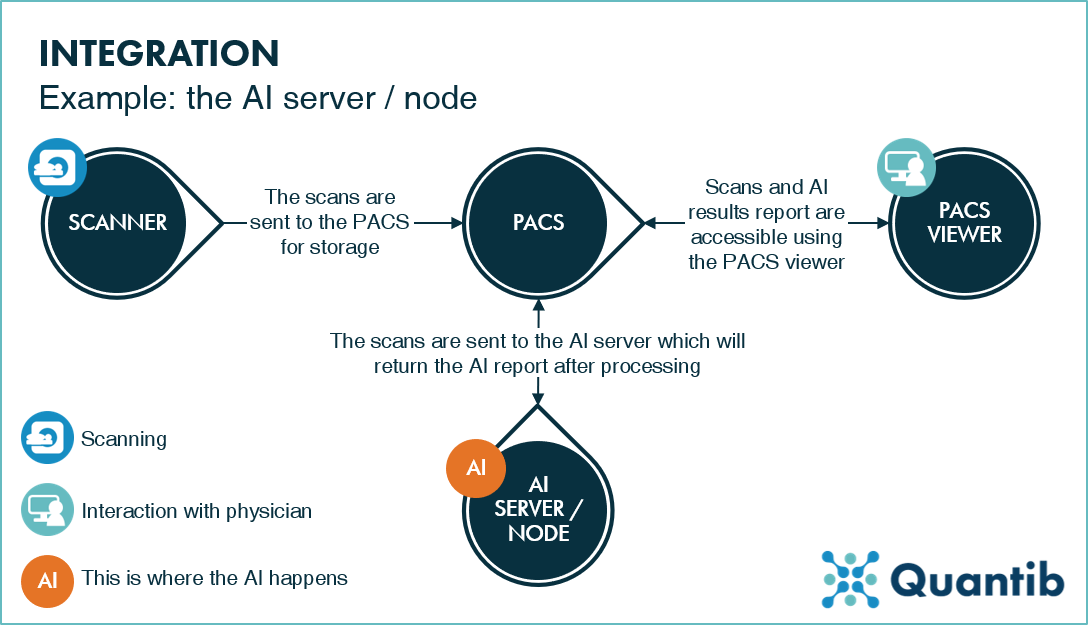 Figure 2: An example of a radiology workflow with an AI node installed. The AI server receives the scans from the PACS, processes them, and returns the results to the PACS, where the results are stored and accessible through the PACS viewer.
Figure 2: An example of a radiology workflow with an AI node installed. The AI server receives the scans from the PACS, processes them, and returns the results to the PACS, where the results are stored and accessible through the PACS viewer.
3. Platform AI integration
Integrating multiple software programs is not easy and generally takes much time. Hence, hiring a company dedicated to standardizing these AI integration processes can be a fitting solution. This would be a platform company. Very briefly, this works as follows: the platform company manages all integrations of AI algorithms with their platform, after which they make a single integration of the platform with the hospital network - an approach very similar to app stores.
For radiologists, it is easy because they can access a selection of algorithms from different AI vendors through one platform. For AI vendors, this is convenient because they only need to integrate once (which should be an easy integration, well-supported by the platform company, as integrating is their core business). For the platform company, it is good because they have got a business.
The downside is that there are quite a few of these companies in business right now, including big vendors such as Philips, GE, and Siemens. So, again, AI vendors need to choose which one(s) and how many to collaborate with.
An example: Quantib® Prostate
Quantib® Prostate is our AI driven solution that provides an intuitive workflow for complete assessment of prostate MRI. It is integrated with Quantib’s dedicated AI platform, Quantib AI Node, to ensure all time access and smooth functioning. At the same time this integration allows the user to have easy access to Quantib’s other AI solutions, such as Quantib ND. The worklist, user interface and report structure of all software packages are similar and therefore easy to work with if the user is familiar with one of Quantib’s products.
The AI node also allows for integration with PACS systems, providing one-click access to the AI Node platform. With automatic forwarding from the PACS in place, the software preprocesses the MRI right after scanning and offers a streamlined workflow from PACS viewer to specialized prostate MRI solution. A standardized and easy-to-communicate report will be created at the end of the reading process and will be sent back to PACS from the AI Node Platform.
Curious to learn more about our AI driven solution? Check Quantib® Prostate.
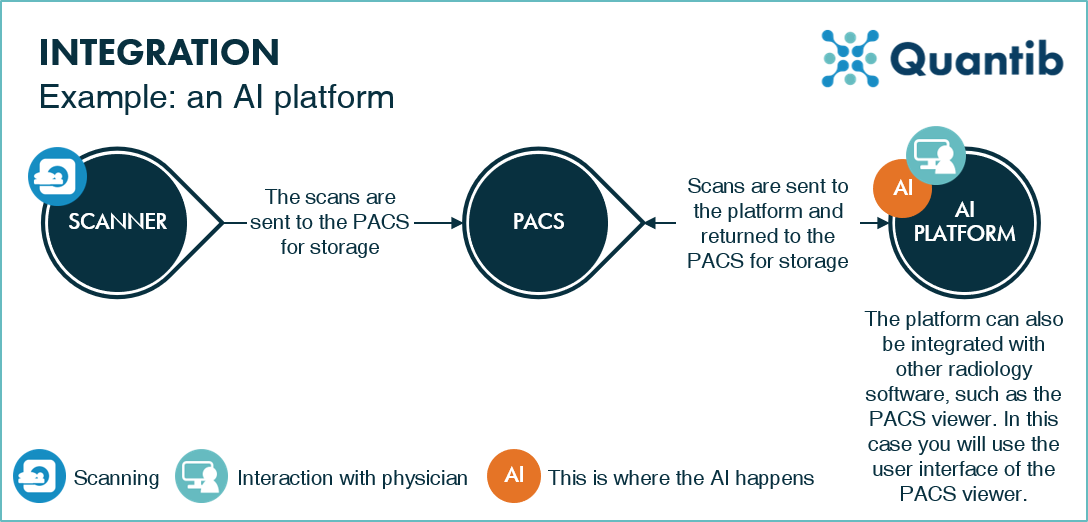 Figure 3: An example of a radiology workflow using a platform. PACS can automatically send scans to the AI platform, which processes them, and shows the AI results.
Figure 3: An example of a radiology workflow using a platform. PACS can automatically send scans to the AI platform, which processes them, and shows the AI results.
4. Tag-along-with-other-vendors AI integration
The radiology workflow already includes a lot of software solutions: PACS viewers, EMR software, a RIS, voice recognition software, and, perhaps, a solution for advanced visualization. AI radiology companies (not part of this list yet) can choose to integrate with other software that has a large, installed base already.
Usually, these types of integrations provide good ease-of-use; the AI software is accessible by the click of a button through the interface of the software that is already installed.
However, implementing this type of AI integration requires a lot of effort from AI companies. Getting the AI software to communicate directly with other software packages can be a tricky puzzle; something that requires time, money, and sincere engagement from both the AI and the radiology vendor that developed the software to be integrated with. Moreover, the trick has to be repeated for other software packages out there. AI companies, therefore, tend to be picky when it comes to integrating with other radiology software vendors.
Upon full AI integration with an established radiology software vendor, nothing major has to change in the current radiology workflow. AI will offer extra support assessing medical images and will simplify drafting the report. Additionally, this situation can provide freedom to adjust and validate the results. At the same time, implementing AI solutions might be a great opportunity to enforce more standardization in radiology. Allowing for too much freedom to edit results will be at the expense of standardization.
An example: pre-filled reports to finalize using voice recognition
Voice recognition is part of many radiology workflows. Integrating AI algorithms with voice recognition software to create pre-filled radiology reports can accelerate the reporting as well as provide a second opinion that is automatically integrated in the diagnosis process. Additionally, it enables standardized reporting as templates to be used for results documentation. An example of such a workflow is shown in figure 4.
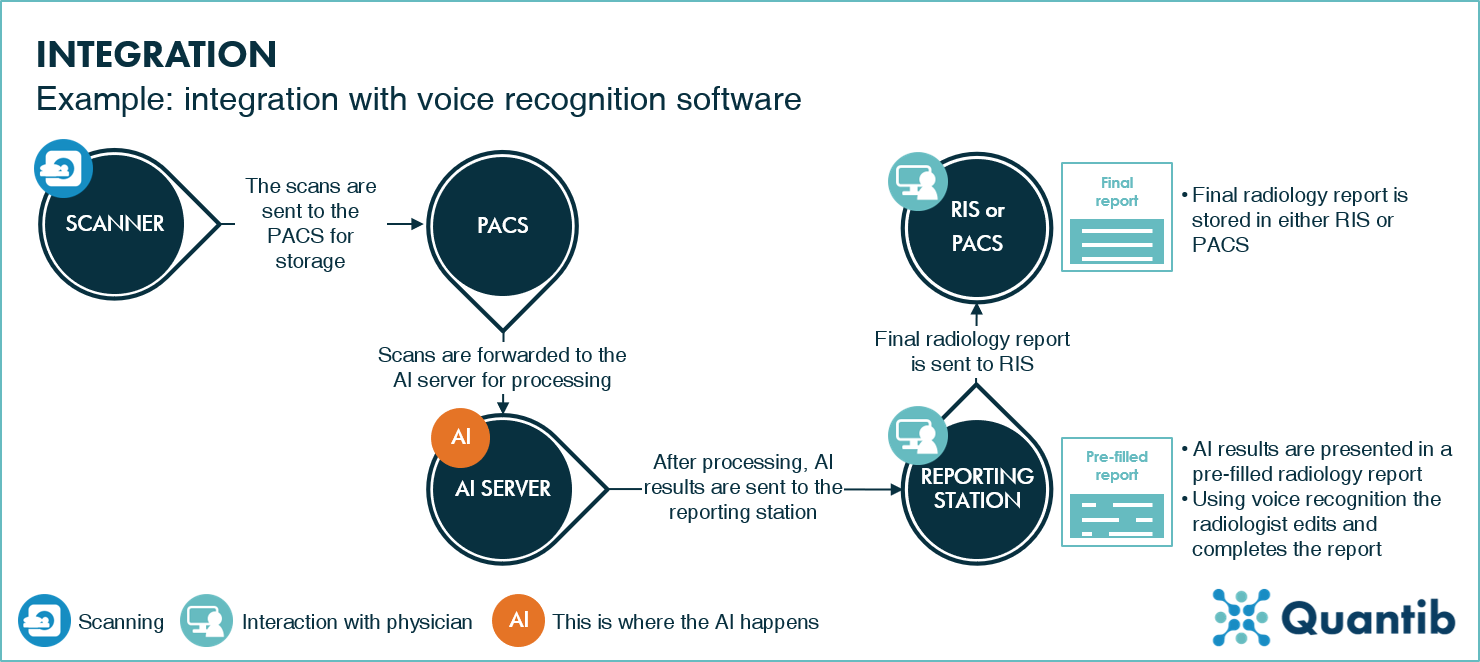
Figure 4: An example of a AI integration in a radiology workflow with voice recognition software. The PACS forwards the scans to the AI server, which processes the scans and delivers a pre-filled report to the reporting station. Here, a radiologist finalizes the report and sends this to RIS after completion. Please note, the exact workflow differs per institute, and the voice recognition software may also push the results to the RIS or the PACS.
5. Multi-department access with AI integration
In the end, radiology results need to make it to referring clinicians. All options described above include AI results in the radiology report which are communicated to referring physicians as a final report. However, another option would be to integrate the AI radiology software with systems that are accessible to other physicians - for example, the electronic medical record (EMR) or the clinical information system (CIS). This approach enables rapid communication and no risk of having inconsistent information in multiple places. However, radiologists will have to settle for having less control over when and how referring physicians see the results.
An example: AI integration into CIS
Integrating AI software with the CIS is not an easy task. The AI server needs to be connected to the CIS, but even more challenging, radiologists need to be able to adjust, or (at least) validate results in the CIS, meaning some sort of user-interface is needed - preferably fully integrated with the CIS. An example workflow can be found in figure 5.
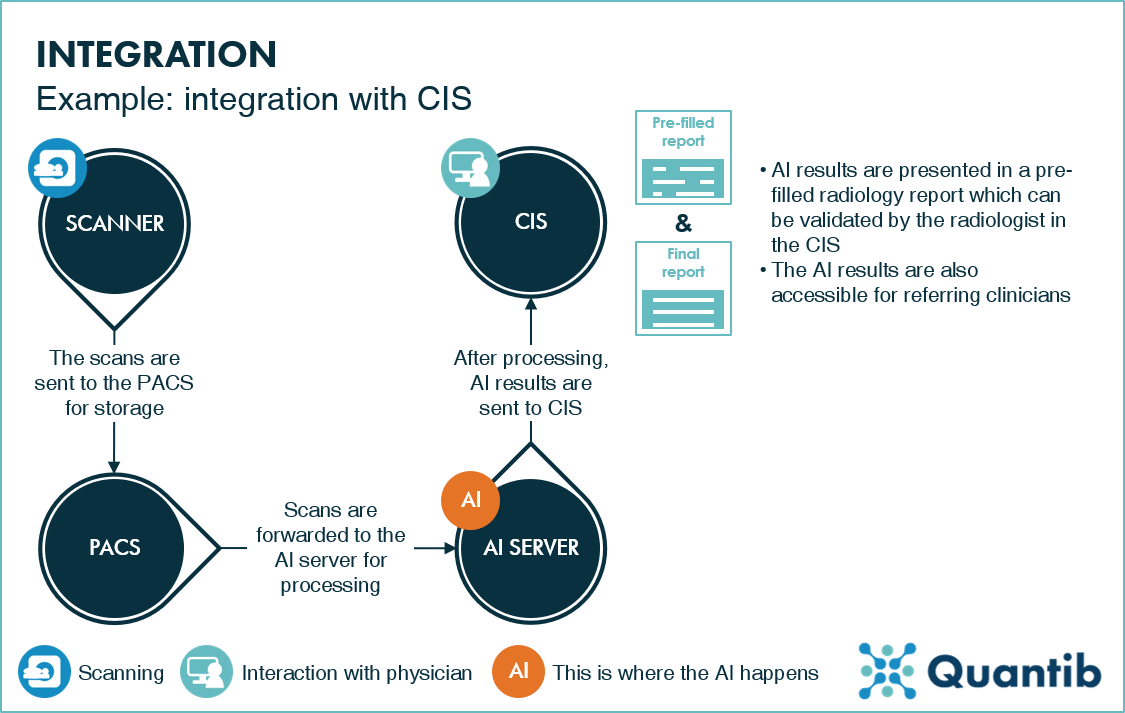 Figure 5: An example of a radiology workflow using AI integrated with the CIS. The AI server receives scans from the PACS, processes them, and pushes them to CIS, accessible for referring physicians, as well as radiologists.
Figure 5: An example of a radiology workflow using AI integrated with the CIS. The AI server receives scans from the PACS, processes them, and pushes them to CIS, accessible for referring physicians, as well as radiologists.
In conclusion
Every approach has pros and cons, and none of them is objectively better than the other. It strongly depends on the situation and the preferences of the institute. An institute with an extensive workload on a specific type of case might prefer a separate workstation, a hospital treating a wide range of different cases might be better off with a platform, or, if the PACS vendor they collaborate with offers an ample selection of algorithms, purchasing this service from their PACS vendor might be the way to go.
Additionally, this article merely discusses a few examples of integration of image-based AI. Artificial intelligence has a vastly more extensive scope of application. AI radiology solutions will include prioritization of urgent cases, filtering out scans without abnormalities, and live scan protocol adjustment based on AI findings on the scans - to name a few. Full AI integration will, therefore, involve all levels of the current clinical and radiology workflow.

